Veterans are at higher risk for Alzheimer’s disease compared with the general population. Part of that has to do with military risk factors like PTSD or brain injury. High rates of diabetes among VA patients also play a role.
That’s why learning new ways to prevent or treat Alzheimer’s disease is a priority for VA research.
One recent study focused on apathy. Apathy is the most common behavioral problem in those with Alzheimer’s, affecting 7 in 10 patients. Apathy involves loss of motivation and initiative, and social withdrawal.
The small pilot study at the Central Arkansas Veterans Healthcare System found that brain stimulation improved apathy. The results are online in the Journal of Alzheimer’s Disease.
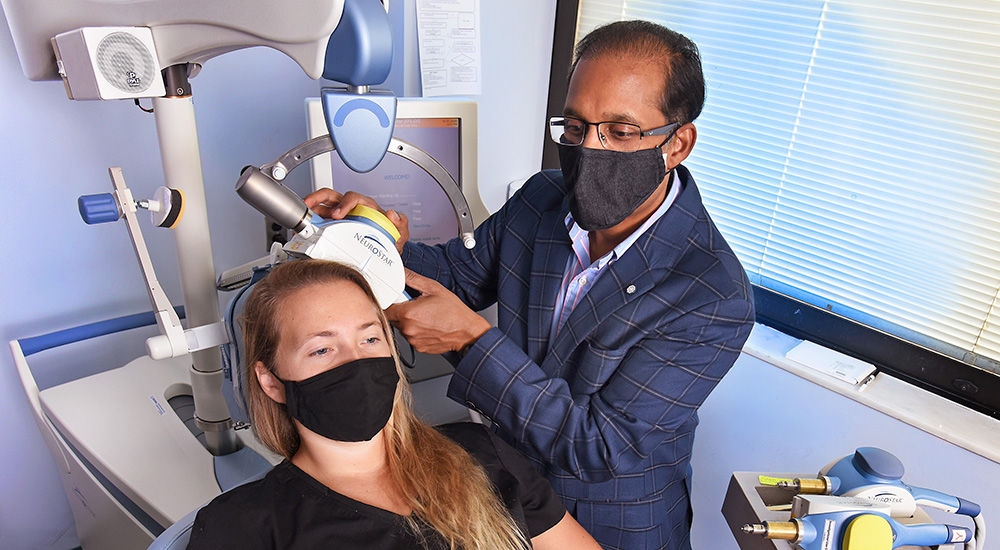
In the photo above, by Jeff Bowen, Dr. Prasad Padala simulates a repetitive transcranial magnetic stimulation treatment with Ashlyn Jendro, a research assistant. She’s holding her thumb up to indicate the twitching caused by the pulses.
Pilot study involved 20 Veterans
Twenty Veterans with Alzheimer’s disease and apathy took part. Half received repetitive transcranial magnetic stimulation (rTMS), a type of brain stimulation. The others received sham stimulation, basically a placebo.
Through patient and caregiver interviews, the VA team documented “significantly greater improvement” in apathy levels in those who received brain stimulation compared with the control group. The positive effects continued up to three months.
Besides improvements in apathy, the researchers also noted “significantly greater improvement” in memory, attention, and cognition in the rTMS patients compared with the sham treatment group.
In rTMS, doctors apply magnetic coils to the scalp at specific points. This creates an electric current in brain cells. The Food and Drug Administration has approved the therapy for depression that doesn’t respond to other treatments. The technology is being studied widely for other brain disorders including Alzheimer’s.
The research team concluded that repetitive transcranial magnetic stimulation “may be safely used in people with Alzheimer’s disease and may improve apathy, function, and some aspects of cognition.”
How long does the benefit last?
Can the effect last longer than three months? “That’s the million-dollar question,” says lead researcher Dr. Prasad Padala. He is a geriatric psychiatrist with VA and University of Arkansas for Medical Sciences.
“Unfortunately, no study has looked at that thus far. Ours is the first study to say that the effects persist until three months. I don’t know about four months. I don’t know about five months. The only thing I can say is at three months the effects were still there.
“If I have to treat somebody clinically based on this result, I would be inclined to give them a maintenance treatment, a booster dose of sorts at three months, like we do now for treating depression.”
Apathy keeps neurons from connecting
The main side effects from the rTMS were discomfort in the area where the magnet sat on the patient’s head, and headaches. Those issues occurred only during treatment and resolved soon afterward.
Padala says those in the study who received the sham treatment were subsequently given access to the real treatment through a clinical program.
He is enthusiastic about the therapy’s potential.
“I’m so interested in this area because people with pre-dementia who lose their motivation and have a lot of apathy tend to convert into dementia at much higher rates than those who keep their motivation and interest levels.
“So if you don’t do anything in your daily life, you’re not connecting the neurons in the brain and you’re hastening the process of neuro-degeneration. To put it simply, if someone has pre-dementia and on top of that they have apathy, their brain shrinks faster.”
Based on his research to date, he believes “brain stimulation may slow down the shrinking of the brain.” More study is needed, he emphasizes.
Topics in this story
More Stories
Pacific Islands VA opens new Akaka clinic in Kapolei, bringing a variety of VA services to Oahu’s leeward side
Veterans can now navigate VA resources with confidence using the new VA Resource Navigator
In this episode of PTSD Bytes, integrated health psychologist Dr. Octaviana Hemmy discusses treatment for HIV and PTSD.






Nearly 4 ears ago, then Presidential Candidate Trump , promised veterans to truly clean up their treatment messes and he has. done so Now read this story and pray the treatment will work longer and longer ad infinitum.
I have been diagnosed with dementia for about six years and, recently, Phase II (whatever that means) Alzheimer’s. I am enrolled in VA Health Care and currently rated at 80% disabled by VA VBA. What are my chances of getting involved in this program in Florida?
I have tried to leave my information and it states: nothing in my Catch a??????
How do I sign up for your memory improvement program?
How can I participate in this study? I have a Foggy memory
I’m afraid my mother died for this condition. I’m retired total permanente. I’m having problems remembering things. I’m US AIR FORCE..