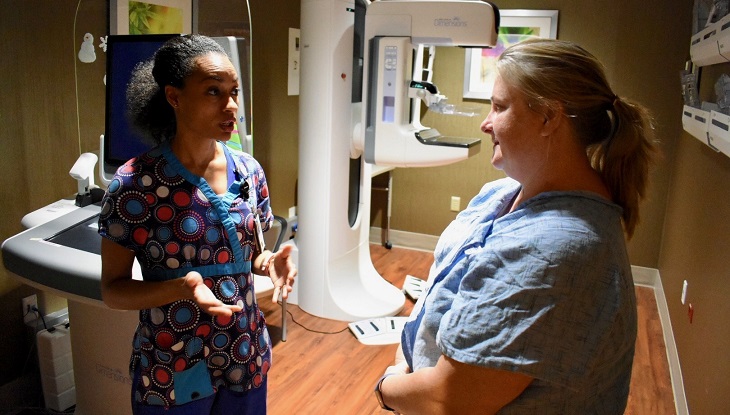Kathy Lowery thought she had visited VA North Texas’ Dallas campus for the last time after she completed a routine mammography screening on December weekday afternoon.
When it comes to routine exams, no news is often good news.
“I got called back after my routine exam because they found something on my mammogram,” said Lowery, a U.S. Navy Veteran. “When I first got the call, I didn’t want to panic and spiral down into negativity, but your mind goes there.”
The stress associated with Lowery’s return to the Dallas VA Medical Center for a follow-up examination could have been disabling had it not been for a team of skilled and caring professionals that perform some 3,400 like exams each year.
A friendly smiling face can make all the difference to a Veteran facing the unknown at a medical appointment.
“I walked into the clinic and they’re so friendly and happy and to see me,” said Lowery. “I felt very welcomed and my stress level subsided.”
The Radiology Team in Dallas has done in-house mammography since 1985, and greatly benefited from substantial system-wide technological upgrades in 2017 that brought Hologic mammography units to serve the 15,000 (and growing) women Veteran patient population of VA North Texas Health Care System. The mammography imaging suite in Dallas provides a spa-like environment for patients with a dedicated private waiting room. Soothing music playing can be heard when entering the suite to help create a calming, friendly setting for the Veterans.
Giving Veterans the very best patient experience for life-saving examinations and treatment is priority number one for the mammography team.
“We go above and beyond to meet the Veteran’s needs so they feel comfortable and confident in their routine exams,” said Marlo Trabue, VA North Texas Radiological Technologist. “Our patients are family and we ensure that they understand the importance of these exams and how early detection can save their lives.”
Clinic patients not only have one-stop access to basic screenings and diagnostic mammograms, but also breast ultrasounds, ultrasound-guided core biopsies, cyst aspiration procedures, stereotactic breast biopsy and needle wire localization under mammography or ultrasound guidance.
And women Veterans aren’t the only patients seen in the clinic. On average, 15 male Veterans are treated each week. Although breast cancer in men is not as common, according the American Cancer Society, in 2019, some 2,670-new case of invasive breast cancer will be diagnosed. Male breast cancer is most common in older men, though it can occur at any age.
“Men diagnosed with male breast cancer at an early stage have a good chance for a cure,” said Trabue.
Early detection through regular self and yearly exams is recommended for most patients, regardless of a family history of breast cancer. For Kathy Lowery, being proactive with her exam was the only option.
“I’m prepared to take any actions needed to be there for my children,” said Lowery.
Thankfully, after her follow-up visit, Lowery learned that she would not have to be seen again for another year.
“I’m thankful that nothing was found after further study,” said Lowery. “But you just never know what can happen and I’m glad that I had I had this VA team to ensure I would continue to be there for my family and children.”

Topics in this story
More Stories
Struggling with setbacks in your fitness journey? Trade discouragement for finding motivation in daily improvement in this week's #LiveWholeHealth video.
VA offer resources and a network of support for all women Veterans including those who do not seek care with VA.
VA can help people balancing caregiving duties with caring for a child and managing personal mental health.