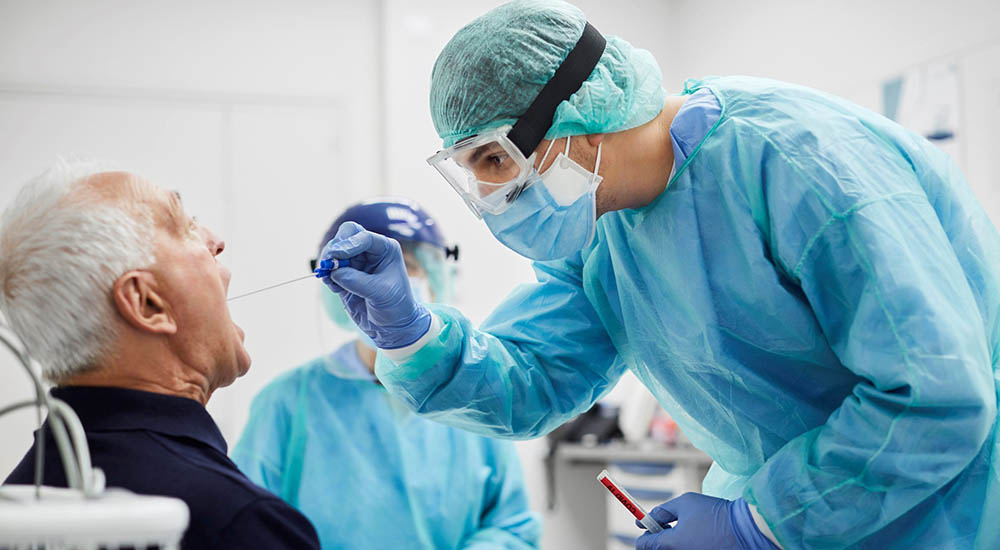
Nurses are talented, versatile health care professionals. They provide expert care, support and professional insight across all health care settings. As with most health care providers, nurses are specialists in their fields. Those field include dialysis, geriatrics, wound care, intensive care unit (ICU), anesthesia, telehealth, diabetes education, mental health and scores of other areas of practice.
Nowhere do we see this expertise more evident than at VA medical centers across the nation. There, over 106,000 nurses care for the millions of Veterans enrolled in VA health care. VA counts on all its nurses, at every level, and their unique skillsets to support care for Veterans and civilians fighting against COVID-19.
Cross trained over 350 nurses
In Philadelphia, at the Corporal Michael J. Crescenz VA Medical Center (CMCVAMC), over 350 nurses cross trained to use their skills and experience in the most effective way during the pandemic. The facility drew staff from primary care, education, procedural units, operating room (OR), specialty clinics, psychiatry, quality management and anesthesia.

Retraining nurses has not only improved patient safety, it has built a more supportive and bonded staff .
As the hospital expanded COVID-19 treatment areas, these staff members were tapped to support the new units. Nursing also redistributed many staff to support screening for COVID-19 at the facility entrances.
Leadership reassigned the nursing staff to support COVID-19 testing for employees and Veterans in secondary screening areas. Those areas include occupational health and pre-procedural testing.
At the onset of the COVID-19 pandemic, leadership developed a training plan to prepare staff for a potential surge in COVID-19 positive Veterans requiring hospitalization. The medical center conducted an assessment to determine where staff would be needed.
Assigned to various hospital units
In addition to employee and Veteran screening at medical center entrances, nurses were assigned to Occupational Health, acute care units for direct care, and the Community Living Center (CLC).
This training plan included instructor-led, e-learning, and experiential learning modalities on targeted care units under the supervision of experienced frontline staff. Employees trained until they were able to perform clinical care independently.
Many nurses were trained in a simulation center consisting of instructor-led learning stations. Topics included donning and doffing (wearing and removing) personal protective equipment (PPE), respiratory care and management, emergency management and equipment management.
Optimizing the Full-Range of Practice Nurses
Advanced Registered Nurse Practitioners (ARNP) are licensed independent practitioners who have completed master’s or doctoral degree programs. They serve in many capacities in health care. Many may examine patients, interpret diagnostic tests, prescribe therapies and medications when necessary and more. By maximizing these nurses’ full licenses and capabilities, especially during the COVID-19 pandemic, VA can optimize the resources of health care facilities and continue to deliver exceptional Veteran care.
Built more supportive staff
Between March and June 2020, Philadelphia conducted over 15 simulations led by experts from the Penn Medicine Simulation Center. Employees indicated they had improved confidence responding to medical emergencies with COVID-19 positive Veterans.
At the medical center, retraining nurses has not only improved patient safety, it has built a more supportive and bonded staff that has grown to appreciate the many roles nurses play in VA health care.
To learn more about VA nurses visit: https://www.va.gov/nursing/.
This blog is courtesy the VHA Office of Communications. It is part of a VA series recognizing 2020 as the International Year of the Nurse and Midwife. More than 100,000 VA nurses work tirelessly every day to serve Veterans in communities across the country. We invite you to show your support for these everyday heroes. Thank a nurse at your next telehealth or in-person appointment!
Topics in this story
More Stories
Black Lab Raisin reminds Veterans of life outside the hospital, brightens their lives with her endless capacity for joy.
VA remains open for business and is closely monitoring the Change Healthcare (CHC) cybersecurity incident.
Take the stress out of travel. My HealtheVet makes preparing for your time away easy with these five quick tips.