Emergency stroke care for Veterans continues to improve thanks to the expansion of VA’s National Telestroke Program, one of the first nationwide telestroke programs in the world.
The program was launched in 2017 to improve Veteran access to stroke specialists.
“In just two short years, the VA National Telestroke Program has grown to provide acute stroke services in over 30 VA medical centers from coast to coast,” said Dr. Glenn Graham, VHA Deputy National Director of Neurology. “We’ve built an extraordinary team of over 20 stroke neurologists across the United States, united in their passion to improve the care of Veterans in the first hours after stroke.
“We’ve developed new technological tools dedicated to the task, such as the Code Stroke mobile app, and have improved the consistency and quality of stroke care in VHA nationally.”
Stroke is the fifth leading cause of death in the United States and the leading cause of serious long-term disability. When it comes to stroke, time is brain! During a stroke, 1.9 million brain cells die every minute. Delaying treatment one-hour ages the brain 10 years.
Treatment of stroke with a clot-busting drug reverses the effects of a stroke and reduces long-term disability. Having a stroke neurologist readily available to guide treatment improves outcomes for stroke patients. However, emergency access to a stroke neurologist 24/7/365 is often limited. Telestroke solves this problem by using technology to bring a stroke neurologist to a patient’s bedside anywhere in the country in seconds.
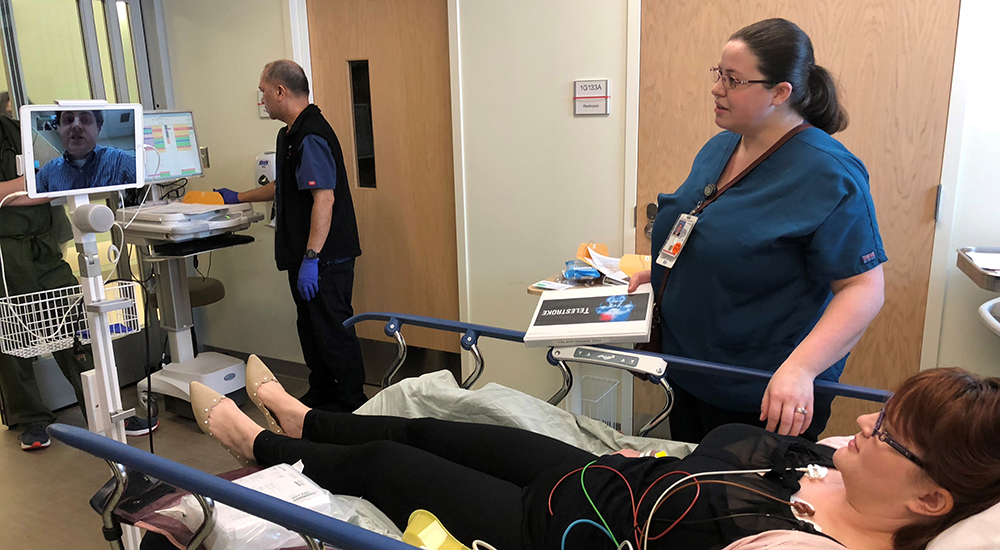
In minutes, stroke victim talking to neurologist via video
The VA program uses an innovative approach to providing services by using low-cost, highly-reliable commercial technology: iPads. When a patient has stroke symptoms, the telestroke neurologist initiates a FaceTime video call to the iPad at the patient’s bedside and has a live conversation with the patient, caregiver, and on-site providers. The neurologist examines the patient, reviews the medical record, and guides treatment.
In the first two years of operation, the program has conducted over 1,000 emergency consults and feedback has been overwhelmingly positive. “Specialty doctors, really good ones, are not able to be in every place at every time. We had a way to connect the doctor with me when I needed it,” said one Veteran.
The program has attracted stroke neurologists from around the country. “It’s the ability to serve Veterans in a new way and to serve Veterans that otherwise wouldn’t get that care, bringing a new service to those areas. It’s been really gratifying,” said a VA telestroke neurologist.
The reach of the program will extend beyond VA with the upcoming worldwide release of the Code Stroke App. The VA-developed app scheduled for release this summer will be free to users worldwide. The app is designed to be used during a stroke code to reduce time-to-treatment by providing real-time information to all team members regardless of location.
“The Code Stroke app focuses on accelerating the episode of acute care by organizing and managing the repetitive aspects of care while providing decision support, structured interaction between neurologist and ICU/ER staff, and automatic documentation,” said William Cerniuk, Director of VA’s Mobile Program.
Need for quick expert decision is critical
“While our initial focus was on small, rural VA medical centers with little or no specialty care in neurology, it is clear that even large, urban VA hospitals can benefit from participating in the VA Telestroke Program,” said Dr. Graham. “This is really no surprise, as with the increase in stroke treatment options, the need for expert decision making at the bedside and without delay is greater than ever. I can imagine a time when all VAs not having a resident or attending neurologists in the hospital at all times will use telestroke to fill these gaps. There is much exciting room for growth, and much important work to be done.”
Call 9-1-1 right away if you or someone you are with shows any signs of a stroke, such as the abrupt onset of weakness, numbness, vision loss, difficulty speaking or understanding, or loss of coordination. Act FAST!
For more information about stroke prevention and treatment, visit the American Stroke Association website at https://www.strokeassociation.org/en/about-stroke.
Topics in this story
More Stories
In this week's #LiveWholeHealth video, learn how to incorporate mindful movement into your day with yoga and stretching to improve posture, reduce stress and boost mood.
VA’s Caregiver Support Program provides Veterans’ caregivers, especially first-timers, guidance and resources.
Healthy Teaching Kitchen offers Veteran patients nutrition knowledge and the guidance and skills to learn how to cook.







VA health and the veterans administration is not any better than it was. Evidently they don’t bother to read executive orders the President puts out. When you file for benefits or the health side of it you get the same story over and over I have even taken people with me to witness the same awnsers over and over it don’t matter if you have Line of Duty showing on your records it don’t matter if you have 5 DD 214’s
It don’t matter if it’s Fedral time or not .
And I am starting to believe if you had a condition while on active duty or training for the national guard if you served you are a veteran Period.
And yet we are supposed to stand for our country and be proud .
Proud of what is what I want to know people getting turned away or it taking 15 people to look at your records and get told the same thing over and over. Some vets including me will probally be dead before they are approved and I just find out after 30 yrs I am eligible for benefits and now here we go again fight for every dam thing I earned.
But it’s still gonna be a dammed good day without the administration it’s a crying shame it works like this but it’s true to the core.
I, Julio Alberto Pacheco an American Citizen/national/Medically Retired Veteran. The article sounds great.
But on July 30, 2017 I had a TIA followed by a Stroke a week later.
When the ER doctor called Martinsburg WV VA Hospital. They refused to take me though:
a. I was one of their patients.
b. I have a rated disability for my heart.
c. Therefore denying me medical treatment for a rated disability.
d. They also REFUSED to send the ER doctor my medical records and the results of the Loop Chip Recorder. Implanted to record my heart rate for 2 years. Due to several black outs. Which caused me injuries that required surgery and left permanent injuries.
From TIA and Stroke I ended up with permanent physical damage and permanent brain damage as a result.