In February, VA’s Veterans Benefits Management System (VBMS) completed a key milestone, electronically processing its 5-millionth claim. It’s a major feat considering how far the agency has greatly advanced its electronic claims processing capabilities in the last five years.
Gone are the days of VBA cubicles engulfed in paper claims. Today, VBA processes nearly 100 percent of disability compensation claims electronically through VBMS. The system allows claims processors and power of attorney designees, nationwide, the ability to instantly review close to 3 billion images related to Veterans claims.
“We use VBMS to manage $60 billion in benefits a year, and it has enabled us to transform the claims process,” said Brad Houston, director of the Office of Business Process Integration, which oversees the program.
Where we’ve come from
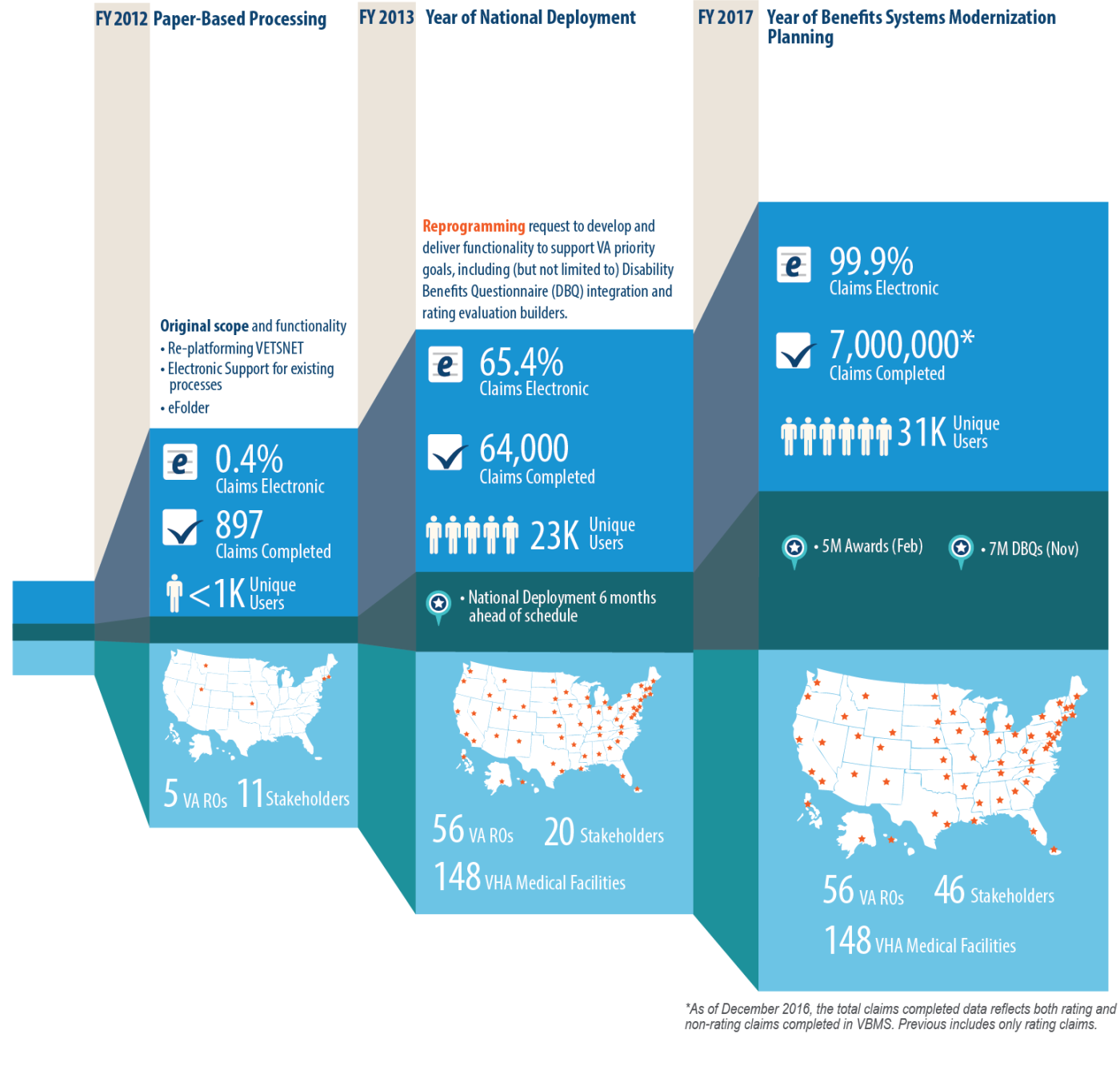
In 2010, VBMS started as a pilot program at the VA Providence Regional Office. It marked the beginning of the Veterans Benefits Administration’s commitment to modernizing its claims processing system. VBMS was pilot-tested at select regional offices between 2010 and 2012, with improvements and greater functionality added to system software releases throughout the testing period. In pilot programs, the then-new system cut the time to process claims nearly in half. By 2013, all 56 VBA regional offices were processing claims electronically through VBMS–six months ahead of schedule.
More work to be done…
In the near future, VBA plans to expand its electronic claims processing capabilities to include automation and digital VA appeal processing, which will eliminate hundreds of thousands of square feet in office-space rent.
“I think Congress made a good investment,” Houston said.
VBMS is one of the many ways VA is striving to be a world-class service provider—establishing a framework for modernizing VA’s culture, processes, and capabilities to put the needs, expectations and interests of Veterans and their families first.
Topics in this story
More Stories
The “Increase Your Credit Score” workshop will be a live event with credit experts whose aim is to help you bolster your credit score and financial stability.
Tax filing season has become a popular time for scammers to target unsuspecting taxpayers through multiple communication avenues. VA wants Veterans to remain vigilant against cyberattacks aimed at stealing personal and financial information.
The VA Health and Benefits mobile app is modernizing how Veterans access and manage their health care and benefits information.






I’ve been waiting since October of 2009 and for the first six month on a person’s desk due to them passing. So now my NOD date was changed to JUN 2010 and now here we are 2017. Yes I believe they are just waiting for me to die before a decision will ever be made.
This blog is just like the VA I wrote a reply of several lines and you rejected the captcha code and erase all I had wrote instead of just giving me the code to do over again!
The VA Claims system is broken and does not look like it going to get fixed anytime soon.
I am a 3 tour Vietnam Medically Retired USAF Veteran. I have been waiting on an appeal for almost 4 years now on my hearing! All my paperwork is correct!
Every time I get a breathing body on the phone at the VA…I am told my case is being worked on!
I guess they are waiting on me to DIE before any decision is made!
The Veterans Administration only works if you know someone “High Up The Chain Of Backlog”
REALLY!!!!!
I was granted 20% disability for Vietnam and Agent Orange in October 2015 and my claim for retired pay has been locked up with the Veteran’s Administration since June 2016 and haven’t heard as word other than about insurance out there for service-connected disease. When would hear a word?
It is just a mess some one needs to get in there and clean it up. I have faith and hope that President Trump will get it fixed because President Obama did not care.
How in the hell can you say Obama does not care? Damn, stop blaming former president Obama for everything and blame the people who are only in it to get a paycheck. I’m so (redacted) sick and tired of everyone blaming Obama.
May tell my story ? I was hurt in a training course back in 1976. I was medically discharges but with minimal recognition for what really happened to me. Rated ten present disabled yet I supposedly only had a contusion in my back. For years I had back pain, sometimes I could not tie my shoes. Some times my leg would go dead on me. In 2009 I had enough, I was able to find a veteran service office that would help me and we ( I ) filed a claim for assistance and Unworkability. My original claim was denied before they even sent me in for an examination. I appealed that denial with the claim of how can you deny the claim before you even set up the examination? That was all messed up, they set me up for ( 4 ) different exams, they then sent 4 letters changing the dates and times. I was told I missed one of the changes and thus, got denied for missing an examination. ( on hearing that I did not request or know they set up ) So I again appealed the denial. This time they set up the examinations and I did attend them. I did get a partial ( win ) they rated me at 70 percent but denied the unworkability. I again appealed the denial for unworkability due to my very limited movement and lifting restrictions. As well as a list of other limitations. Those appeals are November of 2011 and one for May of 2012. They say it is normal for a case to go 5 to seven years. They claim the Record of date is the 2011 & 2012. I and my family still look at this starting in 2009 and counting.
I won my appeal and have been waiting five years for my case settle
Unfortunately the 1-800 # system is Broke also and they just read you a script based on what in the computer. They are not there to Help they are there to just give the script and that is all. I been call for 8 years same answer every time it a joke now when I call if I need a laugh. It be nice if they really wanted to help some one and let you talk to a real case process that has your case. Don’t even tell me about having a designated one as your POA that goes no where with Texas Vet Commission in Waco TX.
I have tried 5 times to get this to go thru. I can never get captcha codes to work…. I have an appeal in from 2008. Went to BVA, sent back to montgmery in sept 2016. BVA told them to get their stuff together, my file has not been updated sence 2014… It does not do any good to call 800 #. All they do is pacify caller. I would like to talk to a person, who can answer my questions. And be able to get things going….
Need a contact person for 3 of my PTSD combat vets to initiate proceedings to begin in the process of making a claim. Also getting in with the correct Primary for care.
These guys can’t even get their ID’s done! Have been told no staff at JBVA Chicago to do this today at JBVA.
I am a retired VA nurse and would like to advocate for them so they don’t run away in hopelessness and no-one to help them.
Please advise asap
JE
I am needing to file a disability claim with the va. My employer put me on total and permament disability 5 years ago. My employer was the Railroad, CSX, This is a goverment disability for PTSD, Bi Polar, Major Depression. Im 51 years old. After reading these post on here, I know now That I will never live long enough to get my VA disability. I served 6 years, 2 overseas, 1 conflict. 19 Delta
I started my appeal in April of 20011 and next month will be 6 years. I think VA just try to forget Vietnam veterans and treat us like when we came back from fighting a war.
My case was filed Oct 2, 2017 as a fast tract. They made it a regular claim even though 90% of the evidence is from the VA med center file. I then requested they decide based on the evidence in the file in Oct 2016. SO they delayed it again and Ebenes says if will be Dec 2017, or 19 months before my case is decided. This is a regular claim, that they tell everyone is supposed to be decided in 125 days, no completed issues at all. SO, the are not really telling the truth in my view about the case backlog.
Here is a suggestion have your treatment Computer talk to your claims computer on service connect treatment received at a VA Clinic or Hospital to update your claim information. Currently this is not happening.
The VA Claims system is broken and does not look like it going to get fixed anytime soon.
Bay Pines Regional Office, St. Petersburg, Fl. The back log of DROs is 27,000 plus, and my number is 24,000, with a 2 year wait list. They process 50 appeals per day, and fail to do 19% right,( IG report). At 71 chances are nill to none. The whole system is in swamp, and 50 years ago, we were fighting in another swamp, different enemy. A typical catch 22, follow, end up where you started, then you die, they win. Can’t fire the union bureaucrats, you will never fix the problem, as Senator Marco Rubio just introduced a bill that does just that, support!!
I appealed and didn’t hear anything. My DD-214 shows the Vietnam medals but found out DD-214 was wrong and had to prove Boots on ground in 67 with being in the 85th Evac hospital in Quinhon Vietnam and an order for glasses. Still getting the run around for 50 years. The Government LIES!
I started with my claim for ptsd in 2001 and the va filled out all paper work. I would appeal, with the va doing it for me with me in the office. Another appeal, I kelp waiting and waiting and went back to see what was happening with my claim and the va rep said it was never appealed, and that person was the same one that filled out the paper work. Now iam going through VA BENEFITS on the internet and every time I try to ck the status I have trouble getting back in ti see if they have even done anything. I just believe that the ca is just waiting on me to die. Now I am 69, and still nothing and I have legitimate claims and seenig Doctor and Psychiatrist. Trying to get things done but can get nowhere. I have a folder 4 inches thick.
nod still have to send in letters to put in file…can not upload anything nod…..still waiting for nod dro iu claim been 17 months …..on nod 2 years from the start waiting….in florida
Ive been waiting 7 years for an answer. They told me I was stuck in a loop and had to wait for it to run its course.The va is so full of (redacted). Ive had claims and my medical records mysteriously disappeared and they made a judgement telling me my injuries dint happen because it wast on file.I had a claim where they sent me to 2 civilian doctors and both said my injuries were most likely caused by the military than not so they sent me to one more doctor, a VA doctor and he said there was nothing wrong with me and never had been anything wrong and the VA threw out the civilian professionals statements and based their decision on this lying VA doctor and denied me benefits. Now Mark what you got to say about that.
Its all true, there has been 4 wars since vietnam and that is old news. the va wants the older veterans to die so they dont have to stand liable for the destruction they caused us.My dad was in world war 2 and he got malaria. there was no cure and told him he would have heart disease at an early age. Well when he was 45 his heart started going out on him, he signed up for disability and they rejected him because there was a fire in the pentagon and the only things that burnt were the ww1 and ww2 military records. there wasn’t any medical backup for his claims.He walked across 7 countries in invasions got out with malaria, jungle rot and the war in his head for the rest of his life, and the government (redacted) on him.He received 3 bronze stars and 3 silver stars and up for the medal of honor, but they didnt care, their only concern was the money they saved by incenerating those files. Would you like to comment on this mark?
Mr. Boyd,
VA’s Enterprise Veterans Self Service (EVSS) portal is not yet capable of supporting a process that allows claimants the ability to complete and submit appeals documentation in an electronic format; however, VA is currently working to build the functionality so Veterans can initiate an appeal and submit all appeals related documents electronically.
Regards,
Mark
Why is the BVA so slow? They have not speeded up., (and don’t give me the answer that they need more personal they have about 1,300 persons per judge) they still take years and years to do an appeal.
Hello Mr. Skidmore,
Once the Board receives your appeal, it assigns it a docket date based on the day you signed your Notice of Disagreement. By law, the Board reviews claims in Docket Date order. Just like at the regional offices, Veterans Service Organizations have offices at the Board and if you have designated one as your POA, they will review your appeal and draft up an argument on your behalf prior to the Board review of the appeal. The Board must also read your entire file and consider the entire body of evidence in your file before making the decision. Their decisions can be quite lengthy and cite legal precedent, court cases, US Code and regulations. Currently, the Board is working on cases with docket dates of January 2013. You can check that date at https://www.bva.va.gov/CustomerService.asp. You may also want to read one of our other blogs on appeals at the Board http://vaww.blogstest.va.gov/VAntage/25855/the-appeals-process-appeals-at-the-board-of-veterans-appeals-board/
I hope this helps answer your question.
Regards,
Mark
Working on docket cases dated January 2013? That’s 4 years ago as it is March 2017. Totally disgraceful.
My appeal has been in since Nov 2011, my hearing was Apl 2013, and just got on the docket Oct, 2016⁉ My brief was not completed and turned in for docket until late Oct, 2016⁉
This is disgraceful !!