National Brain Injury Awareness Month, observed in March, is an appropriate time to remember our Veterans, particularly the wounds they have sustained—both visible and invisible—through their service.
Nearly 1 in 5 among the 2.5 million service members and Veterans who have served in Iraq or Afghanistan since 2003 have sustained at least one traumatic brain injury. The overwhelming majority of these are classified as mild. VA stands committed to improve the lives and long-term health of Veterans with TBI, using a multipronged approach. The effort involves preclinical (lab) research; the development of appropriate therapies; treatment of symptoms such as pain, anxiety, sensory impairment, and memory loss; reintegration back into the community; and caregiver support. This work involves extensive partnerships between VA and both governmental and nongovernmental agencies, and the results can be expected to help not only Veterans, but all Americans affected by this condition.
Transformation Transformation is a powerful word. It denotes rapid, revolutionary change. It is an appropriate word to describe VA research on TBI in the past decade or so. As our nation came to recognize the scope of the TBI problem among service members and Veterans, and as we came to understand, in particular, how many of these brave men and women had incurred “invisible wounds” as a result of their exposure to blasts, VA transformed its small, unfocused TBI research program into a leading, Veteran-centric effort that works closely with many partners, such as the Department of Defense and the National Institutes of Health.
It is noteworthy that over the past 11 years, there has been more than a 15-fold increase in VA Research funding for TBI. The VA TBI research program is focused on service-connected TBI as a chronic condition that can have myriad of co-morbid conditions, ranging from pain and sensory dysfunction to behavioral health issues.
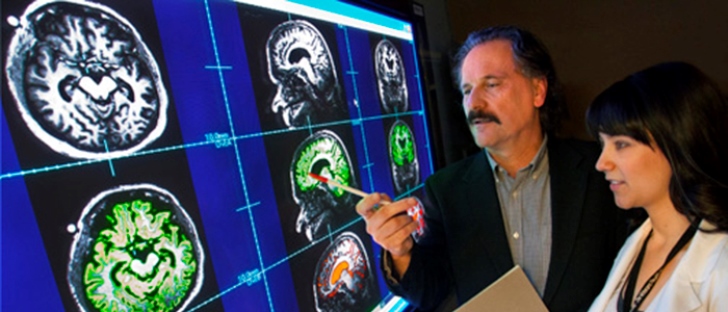
Seeing the invisible TBI has been described as one of the invisible wounds of war, since the majority of these brain injuries are classified as “mild.” The designation is based largely on whether the injury can be detected on a CT scan, but the “mild” label can be misleading. A single mild TBI, or concussion, will cause lingering issues only in a small percentage of people, but many of our Veterans have been injured repeatedly, each incident increasing the risk for long-term symptoms.
VA Research has led the way in developing diagnostics that can detect TBIs that have occurred months or years previously. VA clinicians have been central in the development of neuropsychological tests, such as the Screen and Comprehensive TBI Evaluation, that are being used to help diagnose TBIs in Veterans that were previously undiagnosed, allowing these men and women to receive necessary clinical services to improve the quality of their lives.
However, VA clinicians have realized that there are still TBIs going undiagnosed. Thus, VA Research is funding studies on biomarkers, imaging, and other methods of measuring brain function that should bring better sensitivity and accuracy to brain injury diagnosis.
TBI treatment There are many ways to treat TBI that do not involve drugs. VA Research has developed and validated a number of behavioral-based therapies that help resolve or reduce many co-morbid symptoms associated with the chronic effect of mild TBI. For instance, research has led to better control of pain and insomnia—for example, through cognitive behavioral therapies. This dramatically improves the quality of life in those with these persistent comorbid conditions.
One new area receiving a lot of attention is “electroceuticals.” These treatments involve the use of electromagnetic energies—namely, electricity, magnetism, and light. The first two energies stimulate the brain through classical physiological actions. Electricity is well-known to make neurons produce an action potential, or to “fire,” thus stimulating other neurons and increasing brain activity. Magnetism can induce an electric current as a magnetic field is moved over a conductor.
Light, or phototherapy, can work by two different mechanisms. First, it is theorized that light can directly stimulate neurons, but differently from electricity or magnetism. The light-induced stimulation of neurons focuses on energy production, with the idea that increases in metabolism will result in more brain activity, whereas electricity directly drives neurons to fire, and magnetism induces an electric current that acts on the neurons. A second aspect of phototherapy involves the anatomical pathways between light-sensing cells in the eye’s retina and the brain. A small proportion of these retinal cells extend their fibers not into the visual system, but instead to an area of the brain involved in our internal clocks and regulation of hormones. Use of phototherapy in this manner has been shown to improve sleep (sleep disruption is quite common in those with TBI), and improvement of sleep leads to improvements in other issues associated with TBI, such as anxiety and cognitive problems.
Other therapies do not involve drugs or devices, but rely on patients’ learning or relearning skills so that independent living and reintegration back into the community is successful. This includes life skills such as managing a budget and paying bills, shopping, and, importantly, finding and keeping a job. VA Research has active programs to learn what works best in these areas.
As part of this work, we are exploring how to best offer services to Veterans who live in rural areas where specialized rehabilitation services are almost nonexistent, either through VA or private providers.
Some estimates claim that up to 35 percent of current service members are from rural areas. In these situations, telemedicine and telerehabilitation services are critical, and VA continues to lead in developing these systems. Further technological development will extend the reach of VA clinical expertise to Veterans who in areas where access to medical services is limited.
TBI as a chronic condition Although the damage from a brain injury is permanent, the deficits and dysfunction can be overcome, to a large extent, with rehabilitation and time. That said, it’s important to note that TBI is often not a one-time event. Certain lifestyle habits, such as playing contact sports, can lead to repeated concussions. Concussions can occur during military training, either before or after deployments. Repeated exposures to blasts, as well as motor vehicle and other accidents during military service, can result in a series of injuries over a lifespan that can have additive effects on cognition, behavior, and the ability to perceive sensory information.
To determine if these injuries are having long-term, progressive effects on our service members and Veterans, VA and DoD came together under the auspices of the National Research Action Plan for the Mental Health of Veterans, Servicemembers and their Families to form the Chronic Effects of Neurotrauma Consortium. One main goal of the consortium is to understand the implications that multiple mild TBIs can have on the brain, and to assess the long-term risks, especially as they relate to the progressive condition known as chronic traumatic encephalopathy.
The state of the current knowledge on CTE is still limited. Evidence is building that repetitive brain injury can be a leading factor in the development of this progressive dementia-like condition, which was popularized in the movie “Concussion.” However, the percentage of athletes who play contact sports or combat-experienced Veterans who have been diagnosed with dementia or even mild cognitive impairment is relatively small. With that said, rate of early-onset dementia in the civilian population is still smaller, therefore both the DoD and VA are being proactive in this situation by initiating this consortium to determine if this condition exists, what the cause is, who is most susceptible, and how it can be treated.
VA has come a long way over the past decade in brain-injury research. This work has led to improvements in clinical care, and in the methods we use to do the research itself. However, in the end this is not doing research for the sake of research. Rather, it is about restoring injured Veterans to their highest possible quality of life. We as a nation owe that to our Veterans and their families.
Stuart W. Hoffman, Ph.D., is the scientific program manager and senior scientific advisor for brain injury in VA’s Office of Research and Development.
Topics in this story
More Stories
VA promotes early nutrition intervention for chronic kidney disease with targeted programs like Heathier Kidneys Through Your Kitchen.
VA Research Advisory Committee on Gulf War Veterans’ Illnesses hosting Veteran Engagement Sessions in Phoenix for 1990-91 Gulf War Veterans.
Navy Veteran and president of the American Medical Association got a colonoscopy and encourages other Veterans to do the same.





I believe that Jim Fairfax is the best military artist of all time. He’s a Marine, of course. :),
James (Jim) Toson
mental health help sucks at the va ,i get 10min with a shrink a year,no bull.sam
Hyperbaric Oxygen therapy has been shown to substantially help with healing of TBI and PTSD. I do not understand why the VA is not using this treatment to help Vets.
HI,
I’m a Vietnam era SDVOSB fine art photographer…Maybe the best in the VA System.
My art hangs in many VAMC’s across the US.
Just thought you’d like to know?????
Thanks,
Larry