Okay. You’re in constant pain, so you take a fair amount of meds to help you get through the day.
But what if there was a way to get through your day with less medication, or maybe even no drugs? Would you be willing to give it a try?
If so, the Women’s Pain Management Program at the Salt Lake City VA may be your ticket to a new life. Not a perfect life, nor a totally pain-free one for that matter. Just a better life.
In the photo above, a young Veteran examines a dose of Naloxone, a life-saving medication that can bring you back from the brink of an opioid overdose. It’s one of the many things patients learn about while participating in the program in Salt Lake City.
Fear Factor
“I feared the day I would learn that a patient in my care had accidentally overdosed on prescription opioids,” said Jamie Clinton-Lont, a nurse practitioner who serves as Medical Director for Women’s Services at Salt Lake City. “The thought was paralyzing, and it was this fear that fueled the creation of our pain management program for women. I just knew there had to be a better way to help patients battling chronic pain.”
The nurse practitioner noted, however, that while several women in her program have weaned themselves off opioids altogether, most are still on pain medication.
“But medications are only one piece of the holistic treatment puzzle,” she explained. “That’s why our program emphasizes the other puzzle pieces such as mindfulness, healthy lifestyles, and exercise. These pursuits can help you reduce the amount of opioids you’re taking by diverting your attention away from the pain and toward healthy, productive activities that make you feel better about yourself, and about life.”
The Women’s Pain Management Program is the brainchild of Clinton-Lont and a co-worker, Cheryl Kaye, who launched the program in 2013. More than 100 women are now participating.
Feeling Good
“Our goal is to challenge the patient’s comfort zone, to get you focused on feeling good and finding the life you always hoped to live,” Clinton-Lont said. “This includes opening yourself up to new experiences, making and keeping friendships, and trying new activities you might not otherwise try on your own. Yoga, exercise, and meditation are all a part of that.”
She added: “Chronic pain tends to fade into the background when you’re happy and active.”
Participants in the Women’s Pain Management Program attend a pain education class once every six months. This is where they learn about the meds they are taking and how to take them correctly.
During this class they also get to choose what type of therapy they want to participate in. There are six options: Trauma Sensitive Yoga, Living Well with Chronic Conditions, Managing Stress, Aquatic Therapy, Mindfulness Meditation, and Cognitive Behavioral Therapy. Everyone gets to switch to a different therapy every few months so they can eventually experience all six.
Perception is Reality
“Cognitive Behavioral Therapy is one of my favorites,” said Cheryl Kaye, a clinical pharmacist at Salt Lake City and co-creator of the Women’s Pain Management Program. “It teaches patients how to change their unhealthy thoughts and behaviors, thus changing their awareness of pain and helping them develop better coping skills.”
The pharmacist said the ultimate goal is to help women learn how to lead a meaningful life despite the presence of pain that never really goes away.
“Pain,” she said, “should not be allowed to dominate your life.”
Army Veteran Sharon Shiner, 57, agreed.
“I found that my pain was no longer just a part of my life,” she said. “It was my life. I had quit playing with my grandchildren. I had quit painting. I was getting to the point where I couldn’t see what the purpose of life was.”
Adjusting the Sails
Shiner said she suffers from peripheral neuropathy, which involves damage to the nerves; as well as fibromyalgia, a medical condition characterized by chronic, widespread pain.
“It’s like having the flu,” she said. “Everything aches. And it aches 24 hours-a-day.”
The Army Veteran said the Women’s Pain Management Program has turned her life around.
“They taught me that you have to change your way of thinking,” she said. “You have to look at life differently. You have to learn to live in the moment. They taught me that you can’t control the wind, but you can adjust the sails.”
Shiner said that because she now understands how to adjust the sails, she can once again do things she thought she’d never do again.
“I took up oil painting about eight years ago, and I loved it,” she said. “But then these diseases hit me. Sitting for too long would cause pain. Any movement in my arms would cause pain. I got where I associated painting with pain, so I gave it up. Then, after getting into this program, I realized I didn’t have to get it done all at once. I realized it didn’t have to be all or nothing…
“Now I sit and paint in small increments,” she continued. “I play with my grandchildren for short stretches. And at Thanksgiving I have everyone bring food instead of me doing it all by myself.”
Wear and Tear
“Life just wears and tears on your body,” observed Army Veteran Donnie James, 64. “I’m a nurse at a long-term care facility, so 40 years of lifting people in and out of bed gets you down after a while. Plus I have diabetes, which doesn’t help.”
James said her favorite part of the Women’s Pain Management Program thus far is the class she’s taking on Living Well with Chronic Conditions.
“They teach you to set a goal and work toward that goal every day,” she explained. “For example, I was having trouble controlling my blood sugar. I work three, 12-hour night shifts, so some days I would just come home and go to sleep because I was so tired. I wouldn’t eat. Or worse, I would eat junk and then go to sleep. I was a bad eater. I love cookies and I love Twinkies. So my blood sugars were up and down and all over the place….
“But the class helped me focus on what I needed to do: take five minutes, test my blood sugar and eat something that’s good for me before I go to sleep.”
“It makes you feel powerful, knowing what exacerbates your pain and knowing how to control it.”
James said she also learned how important it is to slow down a bit.
“I was in a bad cycle,” she admitted. “I’d feel pressure to get all these things done while I was awake. So then I’d overdo it and feel even worse the next day. Now I’ve learned that it’s okay if everything doesn’t get done. The world will go on. Those are my words of wisdom now…. the world will go on.”
Not a Believer
“I thought their chronic pain program was a bunch of crap,” said 37-year-old Miranda McClurg, a Marine Corps Veteran. “I didn’t want to do it. I wasn’t a believer. But once I got into the program I realized they weren’t trying to take my pain meds away. They just want to make sure I’m taking them safely.”
McClug said the source of her pain is the surgery she had on her spine about eight years ago. She’s been on and off pain killers ever since.
“Right now I’m taking a class called Managing Stress,” she said. “They teach you that you’re in control of your pain, not the other way around. They teach you about deep breathing, and how being active can increase your endorphins. They teach you to be aware of what your stressors are, because stress and depression make your pain feel worse. They teach you how to focus on a place of well-being instead of your pain. This class really turned me around. I look at my pain differently now.”
The Marine Corps Veteran said she was surprised to learn how life’s simple, everyday challenges can actually intensify any pain you might already be experiencing.
“They taught me that a lot of it is mental,” she said. “Money problems, having a fight with your ex, stuff like that. So when I get stressed I’ll just do some deep breathing, or I’ll do my stretching exercises, or I’ll go outside and get some fresh air. Or I’ll go pet my puppy and talk to him.”
Have a question about VA benefits and services available to you? Contact the Women Veterans Call Center at 1-855.VA.WOMEN or visit them at www.womenshealth.va.gov/WOMENSHEALTH/programoverview/wvcc.asp
Topics in this story
More Stories
In this week's #LiveWholeHealth video, learn how to incorporate mindful movement into your day with yoga and stretching to improve posture, reduce stress and boost mood.
VA’s Caregiver Support Program provides Veterans’ caregivers, especially first-timers, guidance and resources.
Healthy Teaching Kitchen offers Veteran patients nutrition knowledge and the guidance and skills to learn how to cook.

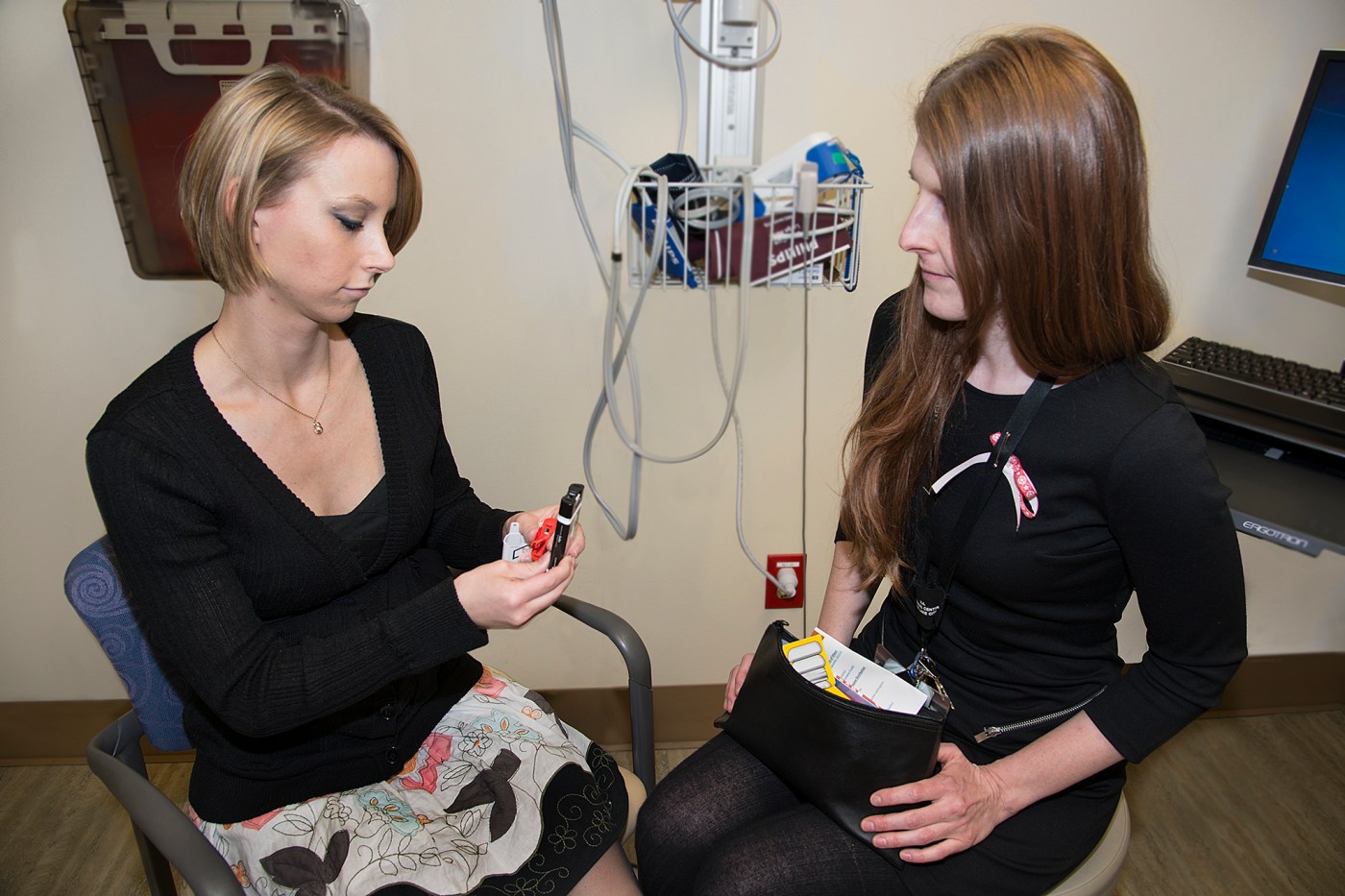







U know male or females we both can have nasty nerve pains anywhere! I have but nerves pain ankle 1981 chemical fire, 2008 va gave a pill resparked the nerves in burn area, pins and needles effect,. I’ve try many thing antidepressants , I get nasty side effect, I don’t know where to go to get help! Va pain clinic sent me to many quacks doctors, one told me I can’t see her more I can’t control my pain, another one use flash cards physical therapy person, did not look or touch it , remember 2nd & 3rd degree burns plus skin gravifting I had i did go thru whirl pool treatment during burn treatment, 30 later I had pins and needles feeling , it went to sleep until I got that pill from va. Va refuses give me any narcotics drug fo pain when it kick in. I know dea rules doctors are puppet s big brother tells them NO NARCOTICS DRUG try other ANTIDEPRESSANTS, which proven does not work.. I even look on internet it comes down final drug is narcotics drug. What on here we all have pain, from war, just dealing with life, so this pain u can not stay it a man or ladies help without be fair .
I don’t know what Female Pain Management Utopia they are running in Salt Lake City, UT; but it couldn’t be further from the truth here in Palo Alto, CA! As a Medical Provider myself, I presented with all my previous Modalities of treatments both successful and failures…1 visit and 9 months of no return phone calls from the Female Pain Clinic, no treatment plan relayed to my Primary Care Physician, not even Patient Advocate could get a phone consult. When I finally had enough I reached out to the Director of the Palo Alto, CA facility and things only became worse. Now, I have been red flagged as “Inappropriate Drug Seeker.” I have been denied reauthorization to Veterans Choice for a “Pain Treatment Procedure” and ABSOLUTELY NO NARCOTICS.
The Women’s Pain Clinic did not offer any of those programs. The Acupuncture program I had tried and even offered to obtain Medical Records. They were determined on one thing and only one thing, to Take Away my Pain Medications, and have told me after Serving My Country as a Medical Officer for 9 years, that if I want Pain Medications for a Severe Back Injury I shall have to purchase a Private Health Insurance Plan because as far they concerned, My Chart is transparent.
U know. 2014 my dr retired from va the np took all narcotics drugs from me . Cold!!!!! I pin needles. In ankle burn I’m choice program after 2 yrs. Found a dr. General doctor he gave me 60 pills I pay for them , this way va can’t do (redacted) about it. Back pain is not fun, va don’t care, did they try give shots in back? Thier some doctors will help a veteran some give pills that don’t work but these doctors get a kick back$$$$$ it happen in all va hospital. I even have headaches know I need ask for that Botox injections but I seen something va try no meds need we can’t do that 375. For the item it show it help vets thier no meds after using it. So va still in pills not new technology . Good luck u get list doctor names find a doc choice program help uuu
VA doctors now talk you out of your pain, or at least try. That is if telling you to learn to live with it and there is nothing else they will do, is suppose to help. A slow painful death is what they offer, with no assistance from the medical community. Using the excuse of the ones who sell their meds, or OD to back them for the latest decision to do nothing for anybody. Our new congress doctors tell the DEA to accuse anyone who lends a hand of being pill pushers and anyone asking for medical assistance is an automatic drug seeker. The pharmacist are the new drug police. What a wonderful world they have imposed on the less fortunate and least able to help themselves. I think they all suck, every time the nerves pinch and cause excruciating pain with most movements. I am sure many are hoping for a merciful end lacking compassionate doctors to help with documented disabilities. All we can hope for is that the ones who have passed this latest round of suffering have a chance to find out for themselves before it’s to late for more unnecessary suffering when there is help available.
Well I totally think a program like this is needed…I allowed the VA to adventally have me taking 260 mgs of morphine a day x 7/8 years I’m guessing…I was an absolute dunder head…to one day it caused my quality of life to be null…after detoxing for 4 1/2 months back in 2013…I found myself still living in a morphine fog…everyday life was a struggle…fog lasted for over a year…wish I had been recommended to a program like this…i now volunteer at our VA in Prescott AZ…I help out a physician that runs a Chronic Pain School…I love it!…and have learned so much once the fog lifted…ha ha…
I am trying to figure why most of the VA clinics treat male & female patients alike. I have a General Practice. She only sees me when I am sick or my physical only. I also see Pain clinic for cortisone injections, physical therapy, GYN, ENT, Mental Health. I see a different doctor for for pain management. I do mind. Why see three different providers for pain in one area. The clinic decided no more pain medications for anyone. The only way is to come in and pee in a cup, wait for the results, then wait for the script
I am curious as to why acupuncture was not included in the Women’s Pain Management Program. The VA Healthcare system highly recommends acupuncture for all types of pain. I am a licensed acupuncturist (and veteran) and treat many veteran patients who come to me for pain relief through the Veterans Choice Program.